Medicaid Planning
Ask us your legal questions
Contact Us
Cape Law
54 Market Street
(Inside Mashpee Commons)
Mashpee, MA 02649
Mailing Address:
PO BOX 2154
Mashpee, MA 02649
Phone: 508-888-8100
Fax: 866-638-8480
A Cape Cod MassHealth Attorney on Medicaid Eligibility

Medicaid, provided in Massachusetts under the Mass Health Agency, is a healthcare assistance program for needy individuals. “Needy,” however, is now a relative term because nursing home costs in Massachusetts average $9000-10000 per month, exhausting a life savings of $100,000 within a year. And while most families hope to preserve their elders’ independence, as a safety measure it is good to learn the qualifications for Mass Health for long term care eligibility as early as possible. Our office streamlines this learning process to help clients weigh feasible options. Below is a 3 point summary of Medicaid eligibility for long term care in Massachusetts.
Eligibility for Medicaid Factor 1: Asset Spend Down
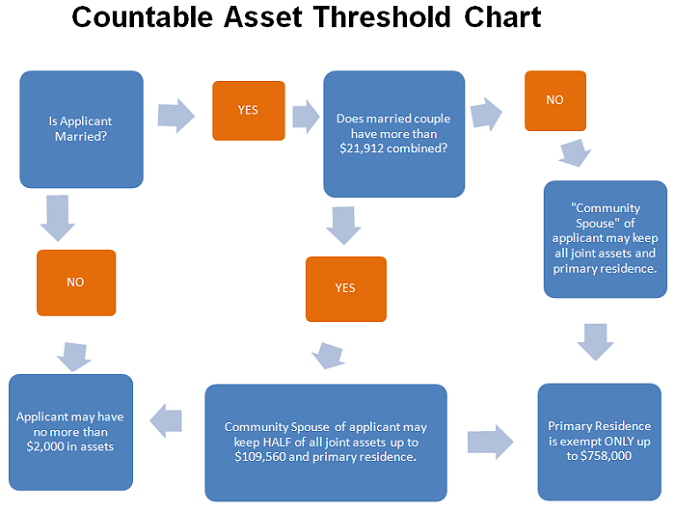
Spending down covers the strategy that an elderly person will take to 1) protect his or her assets, and in the process 2) qualify for Medicaid eligibility. Of course, the earlier an applicant develops this strategy, the more options he or she has available. This is because under the five year Medicaid look-back rule, MassHealth will deny benefits for a penalty period if an applicant transfers assets to anyone other than a spouse, in the 5 years leading up to the Medicaid application. And with $9000-$10000 at stake for each month of a Mass Health penalty, the risk of not planning is pretty significant. So a potential Mass Health long term care applicant should know, as early as possible, what he needs to do in order to secure Medicaid eligibility.
The chart above represents the general asset threshold formula for Medicaid long term care as of 2011. While these asset levels appear small, and they are, part of the service that a Medicaid attorney provides is to help a potential applicant convert his or her “countable” assets into “uncountable” ones. Examples of such conversions include pre-paying for certain qualifying services, or perhaps changing a large sum of money into a stream of income, e.g. to an annuity.
Understanding how to properly execute such strategies, however, takes both experience and legal expertise. While we do help clients that may come to us for help in trying to overcome a denial of long term Mass Health benefits, certain cases are irreversible. Such clients may have attempted to complete the application on their own, or may have received some advice from a nursing home’s business office staff. Understand that such staff may try to help, but they are not hired for their expertise in Medicaid, are not equipped to help convert assets if necessary, and do not generally represent Mass Health applicants in appeals if benefits are denied. Given that 1) a simple mistake resulting in even a month of lost benefits can cost near $10,000, and 2) legal fees are a part of the overall spend down strategy for Mass Health long term care, consulting a Medicaid attorney is encouraged as soon as possible and before starting the application for long term care. This makes the process safer and easier for everyone – for the Mass Health applicant, for the applicant’s family, for the nursing home, and for us! At the very least, check with someone experienced in Medicaid applications before any assets are gifted, transferred or converted.
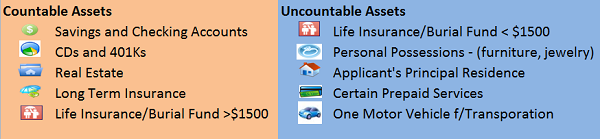
From this table you can observe the general distinctions between countable and uncountable assets. Of course there are other legal and financial instruments (e.g. a trust or annuity) that may be used in addition to guarantee that the applicant and his family can maintain adequate resources after long term care begins.
Eligibility for Medicaid Factor 2: Income
Eligibility for Medicaid doesn’t technically depend on qualifying under a certain level of income, but it is as important to keep these numbers in mind as well when considering your Medicaid planning. All income received by a Medicaid recipient generally goes to the nursing home, but certain deductions related to living expenses are available, meaning that the applicant and spouse can keep that money.
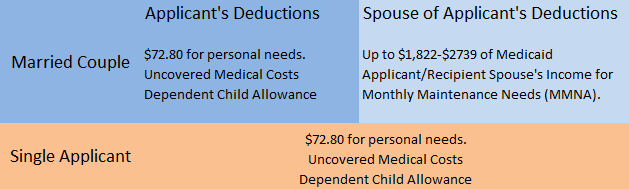
As displayed in the table to the right, a married applicant may deduct certain personal expenses from his income passed to the nursing home, and also those of his or her spouse. The spouse is entitled to a certain amount in order to maintain the ability to live in the community. And so in calculating income for Medicaid purposes, an applicant will take his entire income, subtract his personal expenses, and then subtract any additional amount his wife might need over her own income (up to $1822-2739). This range of potential monthly income deduction from the husband’s income is known as the Monthly Maintenance Needs Allowance (MMNA). The wife’s income will reduce the MMNA she receives from her husband’s income respectively. Again, in applying for Mass Health for long term care a Medicaid expert will help advise you on ways to convert assets into income or vice versa, if such a strategy is needed.
Eligibility for Medicaid Factor 3: Age and Disability
Generally, anyone over 65 falling within the resource and asset requirements described above is eligible to apply for Medicaid for long-term care if they also need assistance with activities of daily living (ADLs) like eating, dressing etc. Applicants not over the age of 65 may also be eligible for long term care under Medicaid, with a showing of severe disability or blindness and limited income or resources.
Topics Covering Long Term Care Medicaid Eligibility in Massachusetts
Clients initiate the MassHealth planning process at different times and for different reasons, but many of them share very common concerns. Below are some resources explaining the more frequently occurring issues we encounter with Medicaid and MassHealth eligibility and planning, for your information:
Protecting the Community Spouse while gaining Eligibility for Medicaid
Spend Down Assets to gain Eligibility for Medicaid
The Five Year Lookback Rule and Eligibility for Medicaid
Tips From a Massachusetts Medicaid Attorney Part 1
Tips from a Massachusetts Medicaid Attorney Part 2
5 Ways a Massachusetts Medicaid Attorney Streamlines the Application Process
Medicaid Fair Hearing Process – After the Mass Health Denial
Ask us your legal questions
Contact Us
Cape Law
54 Market Street
(Inside Mashpee Commons)
Mashpee, MA 02649
Mailing Address:
PO BOX 2154
Mashpee, MA 02649
Phone: 508-888-8100
Fax: 866-638-8480

kf5abi
ip62wv
0ti76h
iaw8g4
31rnv5
936z5j